Featured Presentations
from RESEARCHERS & MEMBERS AT choir
On November 6, 2020, the Osher Collaborative’s Virtual Integrative Medicine (IM) Network Forum convened both within and beyond Harvard Medical School/ Massachusetts General Hospital and its teaching affiliates to build clinical networks, strengthen connections, and provide an environment for seeding new ideas and opportunities. Members of the Center for Health Outcomes and Interdisciplinary Research (CHOIR), formerly known as the Integrated Brain Health Clinical and Research Program (IBHCRP), presented their research to the IM community, showcasing their development for various mind-body interventions.
Live Video Mind-Body Treatment to Prevent Persistent Symptoms Following Concussion: A Study Protocol
Jonathan Greenberg, Phd
Dr. Jonathan Greenberg is a research staff psychologist at the CHOIR, where he studies and develops mind-body interventions for chronic pain, mTBI, depression, and anxiety; and for improving cognition, emotional regulation, and psychosocial wellbeing.
Background
The Toolkit for Optimal Recovery after Concussions (TOR-C) is an innovative (and the first) mind-body program, delivered over live video, that aims to prevent persistent mTBI symptoms in young adults (18-24) with mTBI and co-morbid anxiety.
Methodology
Participants will complete four weekly 45-minute live-video sessions, practicing mind-body skills, cognitive-behavioral strategies, acceptance and commitment skills, and skills for returning to activity. Assessments and feasibility markers will also be collected.
Results / Conclusions
This study will establish necessary feasibility markers and signals of improvement in post-concussive symptoms, anxiety, disability, and fear avoidance in preparation for a fully-powered future efficacy trial of the TOR-C versus a HE-C intervention.
Live video mind-body treatment to prevent persistent symptoms following concussion: A study protocol, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Jonathan Greenberg, PhD.
NF-Web: Protocol & Qualitative Outcomes of An Online Resiliency Program for Neurofibromatosis
Ethan Lester, Phd
Dr. Ethan Lester is a clinical psychologist and post-doctoral fellow at the CHOIR, where he studies, develops, and evaluates interventions for trauma, aging, neurological disorders, and psychiatric illnesses.
NF-Web: Protocol and qualitative outcomes of an online resiliency program for neurofibromatosis, Osher’s Virtual IM Network Forum, 2020. By: Ethan Lester, PhD.
background
The Relaxation Response Resiliency Program (3RP-NF) is an eight-week mind-body program, tailored for neurofibromatosis (NF), that is delivered virtually via secure video-conferencing. Here, the 3RP-NF was adapted to an online self-guided format (NF-Web).
Methodology
Program completers participated in semi-structured qualitative live-video interviews, where experiences regarding the 3RP-NF and adaptations/ suggestions for NF-Web were recorded, transcribed, and coded using an inductive-deductive analytic approach.
Results / Conclusions
Participants reported positive attitudes towards NF-Web, emphasizing social components, accountability, and tech-assisted teaching methods as well as opportunities the program could provide for those with learning, hearing, and vision impairments. Greater preference towards the 3RP-NF format was stated, however participants indicated that they would participate in NF-Web, should the program be offered. Results of the study support a web-based adaptation to the 3RP-NF intervention, representing a timely and viable option to address relevant barriers to current psychosocial treatments (e.g., in-person).
Recovering Together: Feasibility & Emotional Distress Outcomes in Patient-Caregiver Dyads w/ Acute Brain Injury
Sarah Bannon, Phd
Dr. Sarah Bannon is a clinical psychologist and postdoctoral clinical research fellow at the CHOIR, focusing on brain injury rehabilitation and dyadic interventions for patients and spousal care-partners.
Recovering Together:Feasibility and emotional distress outcomes in patient-caregiver dyads with acute brain injury, Osher’s Virtual IM Network Forum, 2020. By: Ethan Lester, PhD and Sarah Bannon, PhD.
Background
At present, there are no evidence-based interventions to prevent chronic emotional distress in patient-caregiver dyads (i.e., pairs), who have acute brain injury. The Recovering Together (RT) dyadic resiliency program — as a feasibility, proof-of-concept single blind RCT — was thus developed to teach resiliency skills (e.g., mindfulness, coping, interpersonal bond) in effort to prevent chronic emotional distress.
Methodology
Both the RT and placebo interventions consisted of six dyadic sessions (two conducted at bedside; four live video post-discharge). Feasibility markers (e.g., ability to recruit), primary outcomes (i.e., emotional distress) and intervention targets (e.g., mindfulness) were assessed at baseline as well as six and twelve weeks later. Efficacy outcomes were analyzed in separate shared-baseline, mixed-model repeated-measure analysis of variance estimated by restricted maximum likelihood.
Results / Conclusions
In this pilot RCT, the dyadic resiliency RT intervention was feasible; and the findings suggest that it may prevent chronic emotional distress in patients and their caregivers following acute brain injury - both independently and interdependently.
Developing a Mind-Body Lifestyle Program for Brain Health Through Inter-Professional Collaboration
Ryan Mace, Phd
Dr. Ryan Mace is a clinical psychologist with a background in mental health and aging; and a post-doctoral research fellow at the CHOIR, where he’s researching mind-body and lifestyle interventions to preserve brain health across the adult lifespan.
Background
My Healthy Brain (MHB) is the first group mindfulness-based lifestyle program (8-weeks, one 90-minute session per week) that promotes multiple behavior changes related to brain health, in older adults with elevated risk for dementia.
Methodology
Mixed-methods data from the ongoing development of MHB is presented through multidisciplinary clinical expertise and patient feedback. Specifically, it highlights results from phase I (e.g., barriers, facilitators, outcomes) that informed adaptations to enhance the program for phase II.
Results / Conclusions
While MHB demonstrated preliminary feasibility and the potential to modify lifestyle risk factors for CD and dementia in phase I, the program can be improved during phase II. Upcoming work will explore: mindfulness skills, live video delivery, and accelerometer watches for objective assessments.
Developing a mind-body lifestyle program for brain health through inter-professional collaboration, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Ryan Mace, PhD.
Developing a Mind-Body Program for Patients with Knee Osteoarthritis, Obesity, and Depression
Developing a mind-body program for patients with knee osteoarthritis, obesity, and depression, Osher’s Virtual IM Network Forum, 2020. By: Ryan Mace, PhD.
Developing a mind-body activity program for older adults with chronic pain and cognitive decline ,Osher’s Virtual IM Network Forum, 2020. By: Ryan Mace, PhD.
Living with Pain: Mediators of Improved Emotional Functioning within a Novel Mind-Body Intervention
Victoria Grunberg, MS
Victoria Grunberg is a clinical psychology doctoral candidate at Drexel University and a pre-doctoral intern at the CHOIR, where she conducts research in areas of mindfulness, third-wave cognitive-behavioral therapy, and psychological emotional distress.
Background
This study explored potential mechanisms (pain catastrophizing, mindfulness, pain resilience) of improvement in emotional functioning, based on previous results from a pilot RCT that evaluated a mind-body activity program for chronic pain.
Methodology
Participants completed baseline and post-treatment measures on emotional distress, pain catastrophizing, mindfulness, and pain resilience for 10-week GetActive and GetActive-Fitbit programs (90 minutes per week). Data was then analyzed via multilevel linear modeling (MLM) through linear mixed-effects models.
Results / Conclusions
Pain catastrophizing explained a large portion of variance in depression and anxiety; mindfulness explained a medium to large portion of the variance in depression and anxiety; and pain resilience explained a small to medium portion of the variance in depression, but not the variance in anxiety.
Live video mind-body treatment to prevent persistent symptoms following concussion: A study protocol, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Victoria Grunberg, MS.
The Effects of a Mind-Body and Activity Intervention for Chronic Pain on Sleep Quality
James Doorley, MA
James Doorley is a clinical psychology doctoral candidate at George Mason University and and pre-doctoral intern at the CHOIR, where he studies mindfulness, mind-body, and acceptance-based treatments for those with chronic pain and sport-related musculoskeletal injuries.
Background
Secondary data analyses tested whether participants experienced significant and sustained improvements in sleep quality over time, following two novel mind-body and activity programs. Mediators of improvement (mindfulness and relaxation) were specifically explored.
Methodology
A single-blind feasibility RCT was conducted that included two novel mind-body and activity programs (GetActive and GetActive-Fitbit). Secondary data analyses from this study was then used to evaluate mechanisms of sleep improvement.
Results / Conclusions
Both intervention groups experienced significant and comparable improvements in sleep quality from baseline to post-intervention, which were sustained at 3-months follow-up. Mindfulness and relaxation fully mediated the improvement in sleep quality.
Live video mind-body treatment to prevent persistent symptoms following concussion: A study protocol, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: James Doorley, MA.
Home Practice Adherence Among Patients with Chronic Pain in a Mind-Body Intervention
Sarah W. Hopkins, MS
Sarah Hopkins was a clinical psychology doctoral candidate at Suffolk University and an advanced practicum student at the CHOIR, where she studied brain health interventions and their effect on disease prevention, recovery and management.
Methodology
Participants were randomized to a mind-body physical activity program either with or without a digital monitoring device (Fitbit). Home practice adherence was then assessed through weekly home practice logs, which reflected participants’ physical activity, responses to relaxation practices, and gratitudes.
Background
This study examines participant adherence to home practice in a pilot RCT of a mind-body physical activity program for chronic pain. It also investigates the association between home practice and primary physical, emotional, and social functioning outcomes.
Results / Conclusions
40.74% of participants demonstrated excellent home practice adherence. However, there were no significant associations between home practice frequency of physical activity, relaxation, or appreciation skills and outcome variables. Hence, more research is needed to evaluate these variables and relationships.
Home practice adherence among patients with chronic pain in a mind-body intervention, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Sarah W. Hopkins, MS.
A Qualitative Analysis of Couples’ Experiences After a Diagnosis of Young-Onset Dementia (YOD)
Mira Reichman, BA
Mira Reichman is post-baccalaureate student and was a clinical research coordinator at the CHOIR, where she studied mind-body interventions for orthopedic injuries, dementia, and other brain-related disorders. Mira is now at a doctoral graduate program in clinical psychology.
Background
This research aimed to inform future psychosocial interventions for people with young-onset dementia (YOD) as well as spousal caregivers (SCGs). A qualitative study was conducted to gather perspectives on psychosocial stressors; and the adaptive coping strategies of couples after a YOD diagnosis.
Methodology
Semi-structured qualitative interviews were performed over Zoom with 23 dyads (PWD and SCG), which covered psychosocial stressors experienced since diagnosis as well as strategies for coping with YOD. Interviews were then transcribed, coded, and analyzed thematically to reveal couple-themes.
Results / Conclusions
Five themes emerged for psychosocial stressors and seven themes for coping strategies, which support the concept of a dyadic psychosocial intervention that teaches healthy coping skills: acceptance, attention, problem-solving, interpersonal communication, cultivation of positive emotions, and meaning.
A qualitative analysis of couples’ experiences after a diagnosis of young-onset dementia (YOD), Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Mira Reichman, BA.
Multi-site feasibility of a mind-body program for adults with orthopedic injuries: study protocol,Virtual Integrative Medicine Network Forum 2020, Osher Collaborative. By: Mira Reichman, BA.
In it together: A meta-synthesis of stress and coping in patients with young-onset dementia and their caregivers ,Virtual Integrative Medicine Network Forum 2020, Osher Collaborative. By: Mira Reichman, BA.
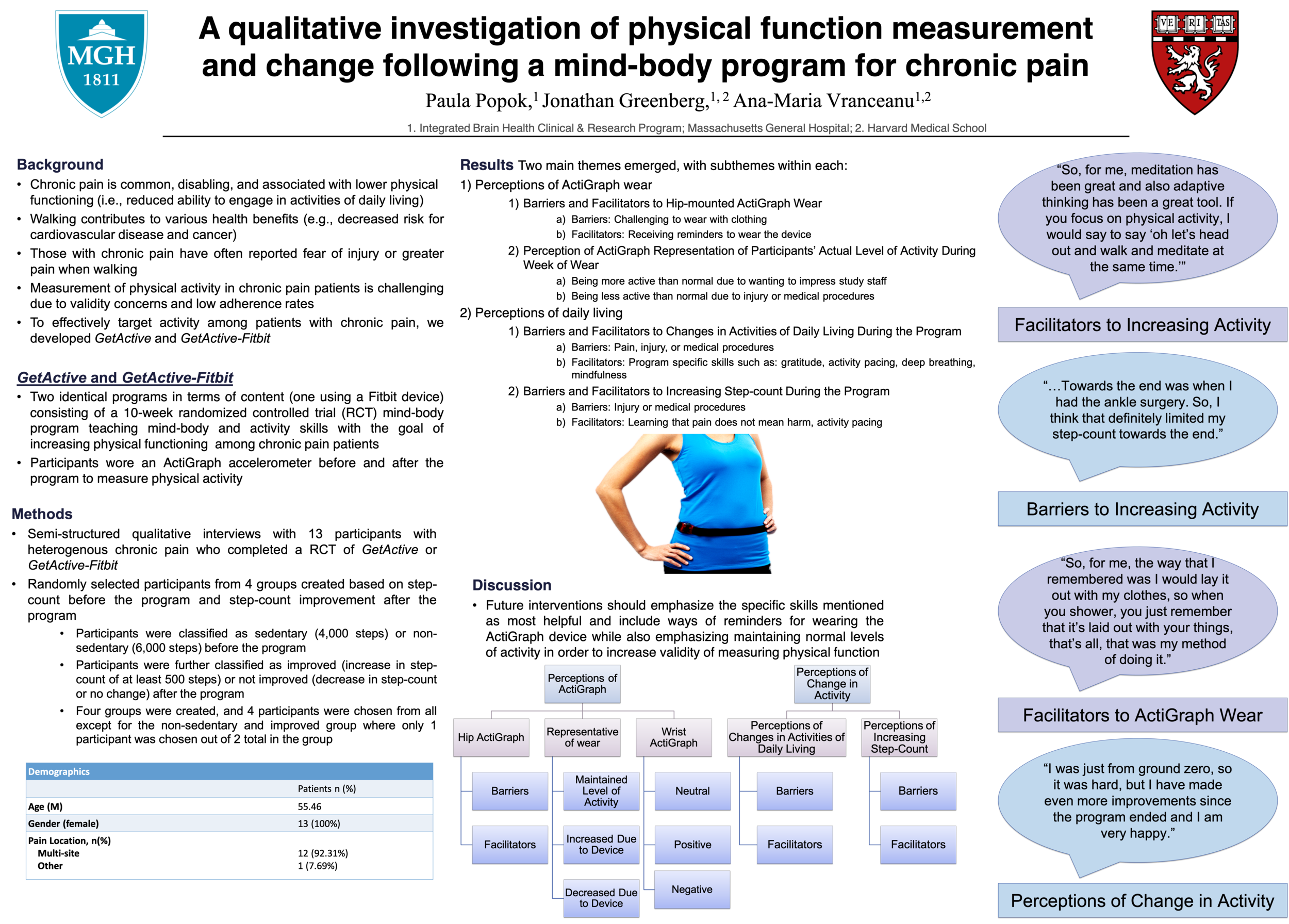
A Qualitative Investigation of Physical Function Measurement & Change Following a Mind-Body Program for Chronic Pain
Paula Popok, BA
Paula Popok is post-baccalaureate student and was a clinical research coordinator at the CHOIR, where she studied biopsychosocial interventions that promote mental health in those with physical dysfunction. Paula is now at a doctoral graduate program in clinical psychology.
Background
This 10-week RCT aimed to effectively target activity among patients with chronic pain via two mind-body programs either with or without a digital monitoring device (GetActive or GetActive-Fitbit). Both programs taught mind-body and activity skills with the goal of increasing physical functioning.
Methodology
Semi-structured qualitative interviews were conducted with 13 participants, diagnosed with heterogenous chronic pain, who completed either the GetActive or GetActive-Fitbit program. Randomly selected participants from 4 groups were also created based on step-count before and after the program.
Results / Conclusions
Two main themes emerged from the study, regarding perceptions of Fitbit wear (e.g., clothing as a barrier; device reminders as a facilitator) and perceptions of daily living (e.g., pain, injury, or medical procedures as barriers; gratitude, activity pacing, deep breathing, and mindfulness skills as facilitators).
A qualitative investigation of physical function measurement and change following a mind-body program for chronic pain, Osher’s Virtual Integrative Medicine Network Forum, 2020. By: Paula Popok, BA.